yahoo Press
Doomed to die, one man chose a risky experiment that changed history
Images
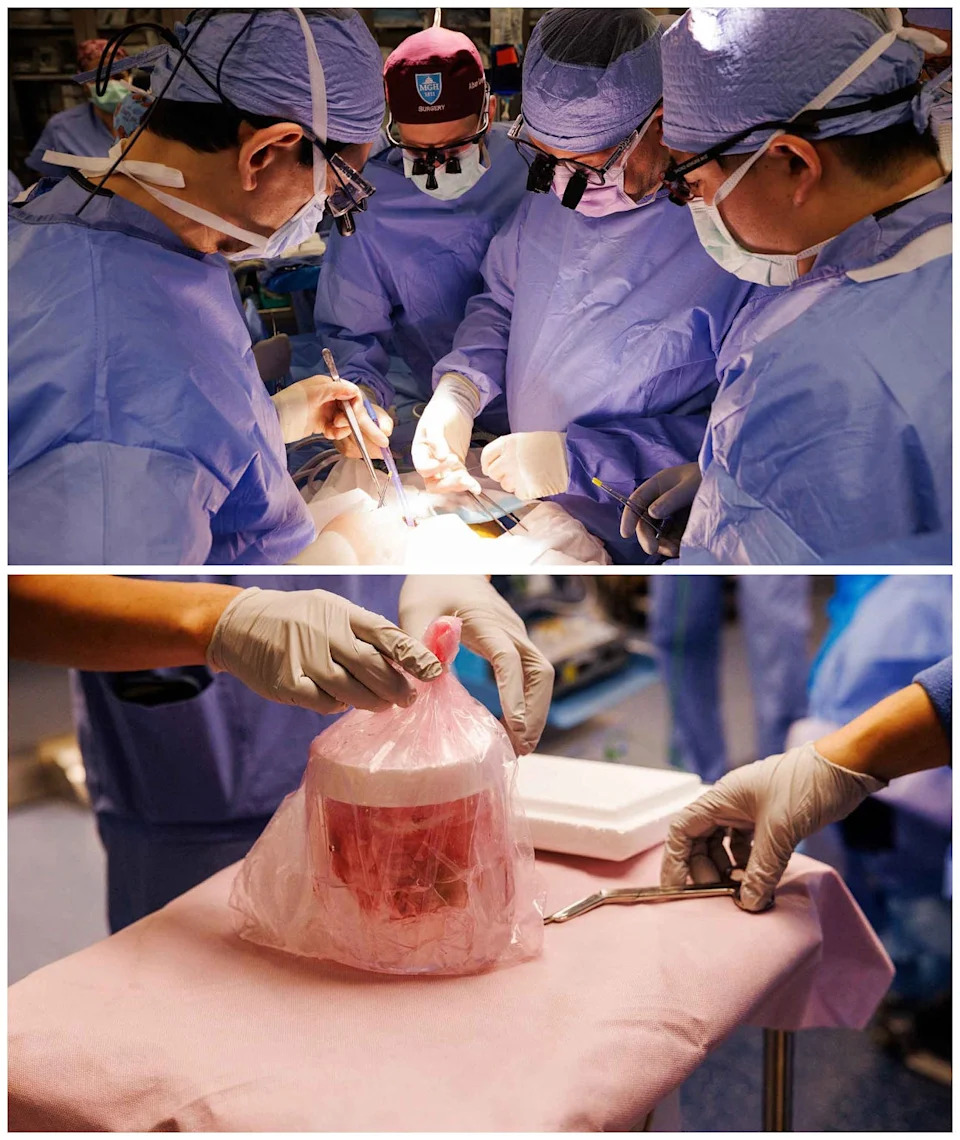
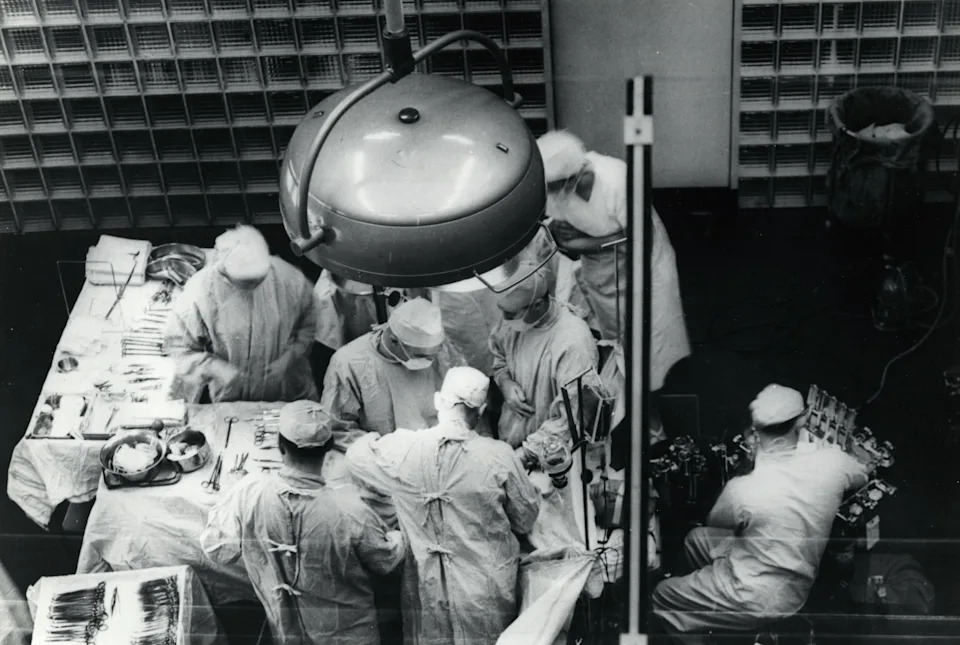
BOSTON ‒ Tim Andrews was so close to death, he was ready to risk what little life he might have left. The retired grocery store manager was told he would have to wait five years before reaching the top of the transplant list and qualifying for a new, life-saving kidney. He knew he wasn't going to make it. Already he could no longer walk or hold down food. So last year, he volunteered for an experimental surgery at the leading edge of scientific research: He agreed to get a pig kidney to replace his own failing organ. "I'm gonna die anyways, why wouldn't I do something for all these [other people with kidney disease] that are suffering?" said Andrews, of Concord, New Hampshire. "I don't care if I die the next day as long as you learn something," he told his doctor. One pig- and one human-kidney transplant later, Andrews, 68, says he is now thinking of his future in terms of decades instead of days. "I'm laughing again," Andrews chuckled, remembering his time as a self-proclaimed "pig man." In the process, Andrews has become an example of how far transplantation has come and what it could look like in the future when there are enough organs for everyone in need and when the medication that enables a transplant’s success doesn’t threaten a recipient’s long-term survival. Andrews’ success as a transplant patient represents a decades-long American journey, one of many USA TODAY is profiling as part of its coverage of the United States' 250th anniversary year. The first-ever successful organ transplant took place in 1954, just a few miles from where Andrews received his own. The distance the field has traveled since −and has yet to go − represents a remarkable and very American medical journey, characterized by big ideas, big risks, perserverence and issues of fairness and eye-popping prices. The result: Andrews is alive and much healthier than he was two years ago. "Oh my God, I'm in a science-fiction movie!" said Andrews, chuckling again, and adding that he's always been a sci-fi buff. "How did I end up here?" More than 100,000 Americans now sit on an organ transplant list, and most of them are waiting for a kidney. Like Andrews, they worry they won't last long enough to get the ultimate gift. For kidneys and some liver transplants, live donation is possible ‒ that is, someone can donate one of their two kidneys or a part of their liver and live out the rest of their lives normally. But not everyone can find a living match among friends, relatives or total strangers. Andrews, like many, eventually benefited from a deceased organ donor. Only about three in 1,000 people die in a way that allows them to donate an organ like a kidney, lungs or heart. The science is getting better, enabling more organs to be used from patients who die older, sicker or further from a hospital. "We're expanding the pool by using what we used to call 'marginal' organs," said Dr. Nahel Elias, surgical director for kidney transplantation at Massachusetts General Hospital, where Andrews had his surgeries. "But at the end of the day, dead people are dead for a reason. Young, healthy people don't just drop dead." And there simply aren't enough organs for the people who need them, Elias and other experts said. That's where the idea of using pig organs comes in. For decades, researchers have been working toward the goal of using animal organs to save people. Some view the trade as unethical, but Americans already eat more than 130 million pigs every year, and pig, cow and even shark tissue have long been used in medical settings. Pig organs are similar enough in size and function to humans', but transplanting entire organs was completely out of reach until about a decade ago when scientists began mastering gene editing well enough to breed pigs whose organs are less likely to be rejected by the human immune system. But xenotransplantation, as it is known, is still very much a work in progress with just 10 Americans, including Andrews, having undergone a transplant. Only six are still alive. Andrews holds the record as of this writing. He lived 271 days with a pig organ. Clinical trials started in 2026 to test pig organs in more people. The goal, doctors say, is to count their survival in years, not days. The advances in organs available and the promise of what's to come are making this "the golden age" of transplantation, said Dr. Shimul Shah, clinical director and chief of transplant surgery at the Mass General Brigham Transplant Center. "It's never been a better time to be in transplantation," Shah said. "Right now, we're blowing up and expanding what we can do. Ten years ago, there was nothing like this." Back in the fall of 1954, doctors were afraid they'd never get organ transplantation to work. Surgeons in Boston had recently tried ‒ and failed ‒ to give 11 people new organs. Those who survived the surgery died when their immune systems rejected the new organs. They had no idea if Richard Herrick's fate would be any different. Herrick, then 23, was in end-stage kidney failure, likely triggered by the scarlet fever he had suffered as a child. Doctors at Boston's Peter Bent Brigham Hospital thought maybe they could get a transplant to work in "Richie," because he had a twin brother, Ronald. No one was sure if the twins were identical or fraternal ‒ there was no such thing as genetic testing back then; James Watson and Francis Crick had only discovered DNA the year before. But surely, they hoped, two boys who had been born at the same time might trigger less immune reaction from a shared kidney. The medical establishment was critical of what the Brigham doctors were considering, with one colleague calling them "a bunch of fools" for even considering the risky surgery. "The whole idea I must admit, was first terribly distressing to me," Virginia Herrick, the boys' aunt, later wrote in The Saturday Evening Post. She and nearly everyone she told about the situation had the same "mixture of horror and pity. Horror at the idea of asking a well, strong young man to make such a sacrifice, when the outcome was so entirely unknown, and pity for the sick brother who seemed doomed to die before he could reach the prime of life." The night before the scheduled surgery, with the boys on different floors of the hospital, Richie sent his healthy brother a note: "You get out of here and go home!" "I am here and I am going to stay here," came the defiant reply. The surgery was a success and both boys were home at the family's dairy farm in western Massachusetts a few weeks later. "There are many hopeful signs that eventually the problem relating to troublesome individual differences may be solved," their aunt concluded, "and that a great many lives may be saved by prompt replacement of a sick or worn-out kidney, or other organ, by a healthy one." Dr. Joseph Murray, the plastic surgeon who led the Herricks' transplant, first got interested in transplantation when he saw World War II victims survive burns with skin grafts. He continued to work on the problem of immune rejection in transplant patients for decades, leading clinical research on medications that made organ transplants possible ‒ first in twins, then between people who weren't so closely related and then from deceased donors. He was awarded a Nobel Prize in 1990. The transplant science Murray pioneered is practiced in every major city in the country and all over the world. But doctors today are still dealing with the challenges of immunosuppression. Every day on the medication that keeps a body's immune system from attacking a new organ, "you're not getting healthier, you're getting closer to developing cancer and heart disease, and eventually it has side effects for the kidneys," said Dr. Tatsuo Kawai, a transplant surgeon and director of Mass General's Legorreta Center for Clinical Transplant Tolerance. The medication that's necessary for survival is toxic, said Kawai, a national leader in finding safer ways to circumvent the body's immune protections. Ronald Herrick, the healthy twin, marked the 50th anniversary of his brother's transplant with Murray in 2004. Richie Herrick had died of a heart attack eight years after his surgery, likely caused by his years of illness. But he did survive long enough to marry his nurse and have two children. Not every person with advanced disease has an equal shot at a new organ, and not everyone in America has an equal likelihood of needing one. Some people lose the genetic lottery and end up requiring a replacement organ, often at a young age. The way the organ donation system is set up, people in certain parts of the country have to be sicker to make it to the top of the list than those in other areas. People with limited access to medical care, exercise and healthy food are more likely to develop diseases that land them in poor enough health to need a new organ. Even making it onto the list can be a challenge. Disease has to be caught early enough for a transplant to make a difference. People who live alone and have no family support aren't considered good candidates for transplantation, and doctors are directed to leave them off the list if they don't meet the qualifications. Andrews' sister Taffy Johnson moved with him into a condo to help with recovery. Without that commitment, the divorcee might not have been eligible for a new organ. Everyone involved acknowledges that the system isn't fair and that perhaps there's no way to make it that way. Still, Jazmin Evans was shocked when told she'd waited years longer for a kidney than she should have. Evans, a Black woman, was diagnosed with chronic kidney disease in late 2011 after a routine high school physical. It was managed with medication for years, but by 2019 she was put on the organ transplant list and started home dialysis, which uses a machine to detoxify the blood, taking over the role of the kidneys. In 2023, the same year she got a successful transplant, she received a letter from the hospital where she'd had her surgery: She should have been able to get it four years earlier. An algorithm used to determine where to put people on the transplant list had been mischaracterizing Black patients since 1999. A faulty study had found that Black people had more muscle mass and therefore more reserves than White people, so they had to be sicker to make it to the top of the list. Evans realized she endured four more years of headaches, crushing fatigue and loss of appetite than if she'd had different color skin. A doctoral student at Temple University at the time, Evans reworked her thesis around what she had learned, focusing on the role of clinical trials and decision-making tools in medical outcomes for Black Americans. "I am hopeful about the direction we're going in," Evans told USA TODAY. "There are people fighting for change. Allowing more perspectives to come into the conversation." But, she adds, "we're not there yet. We still have a very long way to go. (Bias) is an issue that has been plaguing our healthcare system from the beginning." About five years ago, Andrews had been taking care of dementia patients ‒ doing something he felt good about, he said, after 33 years of worrying about "cans of corn on a shelf" as a supermarket manager. He started feeling unusually tired and decided to get checked out. A longtime diabetic, he was diagnosed with stage 3 kidney failure. "It sneaks up on ya," he said. A few months later, his kidneys stopped working completely. "You have 'em and then you don't," said Andrews, who started on dialysis. "You can do the dialysis or you can pick a box. You got no choice." But dialysis "didn't sit well" with him, he said. "Six out of the seven days, you're either recovering or you're sick from it. It's awful, it really is." Medicare picks up 80% of the cost of dialysis, at about $90,000 per person per a year, leaving patients like Andrews to buy supplemental insurance or self-pay nearly $20,000 out of pocket. The U.S. Centers for Medicare and Medicaid spent $6.7 billion on dialysis in 2024; roughly $1 out of every $100 in federal taxes goes to Americans with failing kidneys. About nine months after starting dialysis, Andrews had a heart attack. He was throwing up every day, using a wheelchair because he was too exhausted to walk, and continuing to get worse and worse. "I was a dead man walking," he said. Like the Herricks, he thought there must be something else he could try. Then he saw an article about Richard Slayman, who had received the first-ever pig kidney transplant, at Massachusetts General. Slayman died less than two months after his transplant. Andrews was nervous, but figured he was dying anyway, and some good might as well come from it. He signed on. He did well with the pig transplant. It made him feel much better than dialysis. He was able to hold down food again, including bacon. "Sorry brother, but your taste is so good," he said. But about nine months after the transplant, it stopped working well, and he had it removed. Not long after, Andrews reached the top of the transplant list and a human kidney became available. Amazingly, the person was a perfect match for Andrews' immune system. He's eager to get back to his camp on a pond in Barrington, New Hampshire, about an hour east of Concord. "I'm looking forward to being free ‒ free from my sister," he said, laughing, alongside Johnson, 82. "She was my mother when I was a baby. Now she's still my mother." Andrews chokes up thinking of the pig who gave him a longer life. He named the kidney he received "Wilma" and talked to it. “I tell people I was really sad when I lost her because I was talking to her every day," Andrews said. "You might think that's crazy, but it's not. And, you know, I was encouraging her and she was encouraging me by some of the stuff that she would go through.” He gets even more reflective talking about his human donor. He named that kidney "Spartacus," after the Roman warrior who helped free himself and others from slavery, saying the kidney freed him from the "slavery" of dialysis. "When a human has to die for you to live, that's a lot of responsibility," he said. Back when he was 16, Andrews had signed up to be an organ donor, himself. "Little did I know I would be a recipient," he said. Now, he wants to dedicate the extra years it's given him to convincing other people to be living donors. "If only 1% of New Yorkers would donate, it would solve the problem," he said, on a cold Massachusetts morning, heading into yet another doctor's appointment. The pig kidney transplant didn't cost him anything because it was experimental. But a typical kidney transplant typically runs close to $500,000, with Medicare again picking up 80%. Andrews said he tries not to look at his medical bills, but he received his first denial for other benefits a few months after the second transplant. Still, there's no comparison between the way he felt on dialysis and the way he feels now. It's been a long and rocky journey since he was diagnosed five years ago. But he's gotten to experience so much life. He got to throw out the first pitch at the Red Sox's Fenway Park when he had the pig kidney. He armchair quarterbacked the Patriots in the Super Bowl in February. And he's back to his usual banter with his big sister, a retired nurse who's been living with him to support his recovery. Johnson reminds him about the timing of his medications. "Did you do this? Did you do that? I'm the nag," she said, but then softened. "He'll get into a routine pretty soon. It's getting better. I can see improvement." "I didn't have a brain transplant. I'm still stupid," he replied. "I can attest to that," she shot back. This article originally appeared on USA TODAY: The risky history of organ transplants is filled with American heroes