Press
TSW: Hundreds contact BBC about mystery skin condition
Images
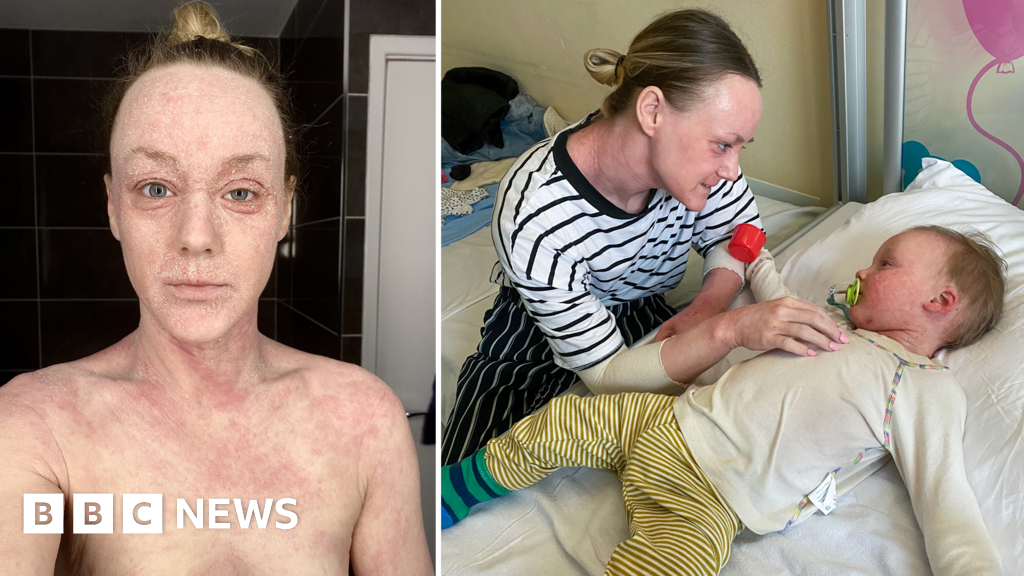
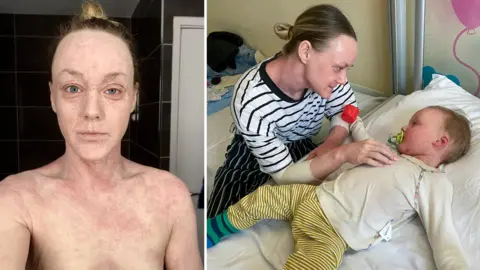
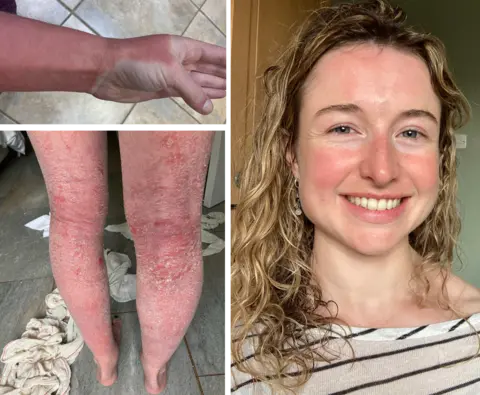
Two weeks ago, I wrote a BBC News article about the impact of a severe and often misunderstood skin condition many people have been sharing on social media, called topical steroid withdrawal (TSW). For some, it's a severe case of eczema. For others, it's a condition in its own right. The problem is doctors can't agree on what it is. The article hit a nerve - millions of people read it and 240 got in touch. So what's going on? I have now spoken to more patients and doctors about why this condition remains such an enigma. In hospital, with her arms wrapped in bandages, Bethany Norman held onto her baby son. He had eczema but, against the advice of doctors, she was adamant he would not have steroid creams to treat it. "Look at what this medication has done to me? Why would I put it on my own son?" she remembers screaming. The 36-year-old believes the creams she was prescribed to manage her life-long struggles with eczema had left her battling with TSW. At that point she had open wounds, a relentless bone-deep itch and her skin would not stop shedding. She says she felt like a prisoner in her own body. There was no way, she says, she would risk her new baby ending up the same way. "I've been told by countless medics that all I have is a severe flare up of eczema and steroid creams will sort it. "They just made it worse." Steroid creams have been used since the 1950s, and have helped millions manage their eczema and live a normal life. They range from mild over-the-counter hydrocortisone to more potent versions available only on prescription. But there is now a group of patients who feel these widely used, safe and effective creams do not work for them. And this is where it can become difficult for medics. In 2021, TSW was recognised by the MHRA, the UK's medicine watchdog, as a reaction to the long-term use of steroid creams - but not as an official condition with a diagnosis and recognised set of symptoms. With research and solutions lacking, there remains deep mistrust between doctors and patients over TSW. "There can be a breakdown of communication," Dr Pippa Bowes, an urgent care doctor in Southampton with a special interest in acute dermatology, explains. "Unfortunately there are cases where patients do not feel believed, and there are medical professionals who are struggling to understand what is going on." Like many doctors, Jenna Crosbie, a trainee GP in north Wales, would have been at a loss as to why a patient like Bethany Norman would refuse steroid creams. Everything she had learned through her medical training had taught her these were one of the first line treatments for eczema. She had been using them to treat her own eczema flare ups for most of her life. The 29-year-old remembers seeing a patient with TSW while working in A&E. "I remember thinking it looked like the most severe full-body eczema I'd ever seen, and I couldn't understand why the patient was refusing steroids," she says. But then, Crosbie began to see her own skin condition change. She had been using more topical steroids to manage her skin flares while working night shifts - but the redness had spread. After doing some more research and realising many of her symptoms were different to eczema, she decided to stop using the creams. Thankfully, she says, her GP was supportive. Jenna now understood what that A&E patient had been going through. "I wouldn't wish it on my worst enemy," she says. Could some doctors be prescribing treatment that in some cases helps fuel TSW? It's a question without a clear answer. Dr Dean Eggit, a GP based in Doncaster, says while steroid creams are vital, they can be wrongly prescribed. GPs, he admits, can often see a red rash and prescribe a steroid cream rather than trying to get to the bottom of what could be causing it. "Unfortunately the beginnings of TSW can look like the original eczema rash in the first place. "So when it comes to treating those patients, there is a risk we keep prescribing them with the creams that might be causing the condition." Guidelines from the National Institute for Health and Clinical Excellence (NICE) recommend a step up and step down approach for eczema, introducing emollients first, then lower dose steroids, then increasing or decreasing the potency as needed. But there are supposed to be checks. Dr Adrian Hayter, from the Royal College of GPs, explains: "If a patient is on a repeat prescription with steroid creams we need to have follow ups and make sure they are using them appropriately." Bethany is among some patients who say they did not receive follow ups and were free to keep using steroid creams as their eczema worsened. "I've seen 30 different doctors and not one believed me when I said the creams had stopped working," she says. "I was being prescribed the strongest potency, I was rubbing it on the affected areas but within minutes the inflammation was back." While there are no NICE guidelines on how to to treat TSW, Hayter says he and other GPs within the college acknowledge it does exist and requires specialist care. Other doctors don't think TSW exists. One dermatologist was so incensed by my article he told me it had left him with a "feeling of absolute dread and trepidation" about how he was going to manage his Monday morning clinic. While he empathised with any patients struggling with eczema, he worries patients are so "consumed" with the fear of TSW, in his view "largely driven by social media", that they are turning down treatments that would help them. Campaigners would like TSW to be recognised by NICE as a condition in its own right, which would give doctors clarity on how to treat it and help settle the medical debate over its existence. But more research is needed over the coming years. Through her own PhD research at the University of Nottingham, funded by the National Eczema Society, Bowes is trying to get to the bottom of why TSW has become so difficult and divisive. By collecting experiences from patients and doctors, she is hoping to create a consultation tool - with a potential set of symptoms and early warning signs - to help navigate this tricky condition. "We do not have all the answers yet, we are only just beginning to understand some of the underlying causes of TSW," she says. Crosbie, the trainee GP, has gained a valuable insight into the condition through her own experiences. Eventually, after 16 months, her skin improved and resolved without any medication, a pattern she says doctors would not normally expect to see if it was severe eczema. All the medics I have spoken to do not wish for a return to the time before steroid creams, as they know they are a vital lifeline for the millions of people who use them without problems. A range of options are emerging for treating eczema. Alongside steroids and emollients, there are immunosuppressants; newer drugs which modify the immune system; and phototherapy which uses UV light. All come with side effects, so doctors say it's important to discuss treatment plans carefully. Albie is four years old now, and Bethany Norman has never applied steroid creams to his skin. She says her son has small patches of eczema which have not spread and is a "happy, bouncy little boy". She has been medication free for a year and says she still gets flare ups but that her condition is improving. What could have helped her when she was in, as she puts it, "TSW hell"? "Being believed," she says. "Acknowledge our pain and try to understand it."